Primary Open-Angle Glaucoma (POAG)
- Dr Andrew Matole, BVetMed, MSc

- Jun 12, 2023
- 10 min read
What is Primary Open-Angle Glaucoma?

Primary open-angle glaucoma (POAG) is a chronic eye condition marked by progressive damage to the optic nerve that, if ignored, can lead to blindness or vision loss. It is the most prevalent type of glaucoma and is commonly referred to as "the silent thief of sight" since in its early stages it generally progresses slowly and without noticeable symptoms.
What predisposes animals to Primary Open-Angle Glaucoma?
Aqueous humor outflow routes become blocked due to inherited abnormalities in the gene that regulates the production of the protein myocilin in the ciliary body and trabecular mesh work.
Primary open-angle glaucoma is epidemiologically connected to certain breeds within a particular population aged between 3 and 6 years of old. Majority of Beagle, Norwegian Elkhound, Petit Basset Griffon Vendeen, Sharpei, Basset Fauve de Bretagne, and Basset Hound breeds are predisposed to this problem.
Breeds of dogs predisposed to primary open-angle glaucoma
Open-angle glaucoma risk can also be influenced by baseline vascular risk factors, such as decreased systolic blood pressure and decreased systolic, diastolic, and mean ocular perfusion pressure. Low ocular perfusion pressure specifically doubles the risk of glaucoma. Cardiovascular disease is one of the significant baseline indicators of open-angle glaucoma development.
What are the clinical signs of Primary Open-Angle Glaucoma?
The clinical signs are often insidious and chronic in onset meaning the disease can go unnoticed for several months. The following are the common clinical signs:-
Bilateral globe enlargement,
Lens subluxation,
Visual deficits or loss,
Corneal changes or disease,
Optic nerve head cupping.
Raised intraocular pressure,
Pain.
How does Primary Open-Angle Glaucoma Develop?

The flow of aqueous humor from the ciliary body through the pupil and into the anterior chamber is seen in this anterior section of the eye. The aqueous humor then goes from Schlemm's canal through the trabecular meshwork into the episcleral venous system. Just below the trabecular meshwork, a smaller amount of aqueous humor exits the eye through the face of the ciliary body (Kwon, et al., 2009).
The ciliary body and trabecular meshwork, the two ocular structures that control intraocular pressure, are among the tissues that produce myocilin. This implys that mutations of the myocilin gene (MYOC) encode a protein that alters the trabecular meshwork and other microscopic features of the typically normal-appearing iridocorneal angle. This results in abnormalities of the extracellular matrix (ECM) changing the aqueous humor outflow pathways and abnormal function of trabecular cells. The extracellular matrix (ECM) which provides resistance to aqueous humor outflow thus becomes pathological in primary open angle glaucoma and intraocular pressure gradually rises. The changes to ECM constituents include reduction in hyaluronic acid and chondroitin sulphate and the presence of an undegradable glycosaminoglycan-like material. Fibrillin in particular may be a major component of resistance for aqueous humor to traverse the trabecular meshwork. As intraocular pressure rises, chronic changes of globe enlargement (buphthalmos) and lens subluxation occur.

The ADAMTS10 gene, which is part of the ADAMTS (A Disintegrin And Metalloproteinase with Thrombospondin Motifs) gene family, produces a protein known as "A Disintegrin And Metalloproteinase with Thrombospondin Motifs 10" that is mainly expressed in connective tissues like the skin, skeletal muscle, heart, and lungs. Extracellular matrix (ECM), which gives different bodily tissues structural support, is formed and maintained by it. It is assumed to have a specific role in the assembly and organization of ECM constituents like collagen and proteoglycans. In the Beagle and Norwegian Elkhound, primary open angle glaucoma has been linked to mutations in the ADAMTS10 gene.
All impacted dogs carry the corresponding mutations in homozygosity.


Retinal ganglion cell axons normally exit the eye through the lamina cribrosa and only become myelinated in the postlaminar area of the retina and optic nerve head. Glia in the optic-nerve head and retina, such as astrocytes and microglia, are inactive. Retinal ganglion cells are stressed as the intraocular pressure rises, and glial cells react aggressively. The lamina cribrosa's retinal ganglion-cell axons get damaged as a result of the generation of a variety of substances, including cancer-causing factors. Increased intraocular pressure is also associated with the production of these chemicals. At this point, no clinically discernible alteration to the optic-nerve head's cupping is noticed.

Apoptosis, or cell death, occurs after retinal ganglion-cell axons are damaged. The nerve-fiber layer becomes thinner as a result of the loss of retinal ganglion cells and axon fibers. With greater cupping of the optic-nerve head (black arrows) and thickening while bowing posteriorly, the lamina cribrosa itself undergoes modification. Apoptosis and neuroinflammatory processes cause cell death and the loss of the majority of retinal ganglion cells and axons in the advanced stage of glaucoma. The lamina cribrosa grows thinner and more posteriorly bowed (blue arrows), significantly attenuating the prelaminar tissue, which causes the optic-nerve head to cup noticeably (black arrows).
How is Primary Open-Angle Glaucoma Diagnosed?
Initial diagnosis of primary open-angle glaucoma is based on the client's description of the dog's bulging eyes that are hazy, and decreased vision. At the clinic, the patients present with corneal clouding, vision impairments, and bilaterally enlarged globes.
Subsequently, the clinical indicators found during an eye (ophthalmic) examination include: -

Globe enlargement: Chronically high intraocular pressure causes the globe's tunic to stretch.

Lens subluxation: Lens zonule stretching or disintegration due to globe enlargement results in lens subluxation and phacodonesis (lens trembling).

Corneal oedema: Oedema of the cornea is present but less severe than it is in closed angle glaucoma. Chronic alterations, such as corneal vascularization and linear striae (breaks and strains of Descemets membrane), are more frequent.

Optic nerve head cupping: The optic nerve head recedes as a result of persistently high intraocular pressure.

Loss of vision: Affected eyes typically preserve vision until quite late in the course of the disease.

Pain: Blepharospasm, sadness (depression), and sluggishness (lethargy) are signs of pain in primary open-angle glaucoma.
The fact that affected dogs respond well to NSAIDS and that it is harder to detect than closed angle glaucoma in dogs suggests that the condition is painful.
Diagnostic investigations
Diagnostic investigations involve Ophthalmic (eye) examination, Tonometry and Gonioscopy.
Tonometry
Tonometry is a medical procedure used to measure the pressure inside the eye, known as intraocular pressure (IOP). It is a vital test in the diagnosis and management of conditions such as glaucoma, which is characterized by increased IOP and can lead to vision loss if left untreated. Tonometry is typically performed as part of a comprehensive eye examination, and it helps eye care professionals assess the risk of developing glaucoma, monitor the effectiveness of glaucoma treatment, or screen for other eye conditions that may cause elevated intraocular pressure. It is a safe and relatively straightforward procedure.

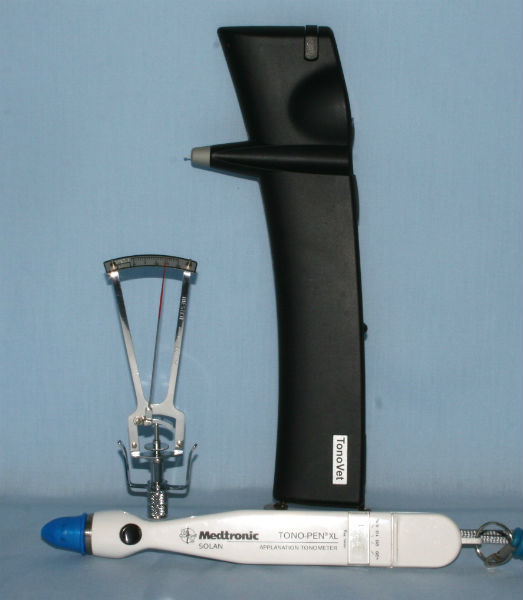
There are several methods of tonometry, but the most common ones are:
1. Applanation Tonometry: This method involves gently touching the cornea (the clear front surface of the eye) with a special device called a tonometer. The tonometer measures the amount of force required to flatten a small area of the cornea, and this measurement is used to estimate the intraocular pressure.
2. Non-contact (or Air-puff) Tonometry: In this technique, a machine releases a quick puff of air onto the cornea, and the change in corneal shape caused by the air puff is used to calculate the intraocular pressure. It is a quick and painless method that does not require direct contact with the eye.
3. Tono-pen Tonometry: This method involves the use of a handheld device called a tono-pen, which is gently pressed against the cornea to measure the intraocular pressure. It is commonly used in situations where other methods may not be feasible or when frequent measurements are required.
Tonometry calibration table
Schiotz scale reading IOP (mmHg) 5.5 gwt IOP (mmHg) 7.5 gwt IOP (mmHg) 10.0gwt
0.5 46 61 75 1.0 44 59 73
1.5 43 56 70 2.0 40 53 66 2.5 33 47 61 3.0 26 40 55 3.5 23 35 49 4.0 21 32 44 4.5 20 29 41 5.0 19 27 38 5.5 18 26 36 6.0 17 24 33 6.5 16 23 31 7.0 15 22 30 7.5 - 20 28 8.0 14 19 27 8.5 13 - 25 9.0 - 18 24 9.5 12 17 23 10.0 - 16 22 10.5 11 15 21 11.0 - - 20 11.5 10 14 19 12.0 - 13 18 12.5 - - 17 13.0 - 12 16 13.5 8 11 15 14.0 - - - 14.5 - 10 14 15.0 7 - 13 15.5 - 9 12 16.0 - - - 16.5 6 8 11 17.0 - - 10 17.5 - 7 - 18.0 5 - 9 18.5 - 6 - 19.0 - - 8 19.5 - - 7 20.0 - 5 -
The normal range of intraocular pressure is 10-25 mmHg with acute glaucoma cases often having IOP >50mmHg. The abnormal eye intra-ocular pressure is always checked by comparing with normal fellow eye.
Gonioscopy.
Gonioscopy is a diagnostic procedure used in ophthalmology to examine the anterior chamber angle of the eye. The anterior chamber angle is the area where the cornea (the clear front part of the eye) and the iris (the colored part of the eye) meet. It is an important area in the eye as it is responsible for draining the aqueous humor, the fluid that fills the front part of the eye.
During a gonioscopy, a specialized lens called a gonioscope is used to view the angle and the structures within it. The gonioscope is typically a handheld lens with mirrors or prisms that allow the doctor to see the angle without obstruction. Prior to the procedure, the patient's eye surface is numbed with topical anaesthetic eye drops, and a gel or liquid is applied to the eye to improve the contact between the lens and the eye.
Then, a goniolens (such as a Koeppe or low vacuum Barkan) is filled with fluid before placing on the ocular surface. The opening to the iridocorneal angle is then viewed with the aid of magnification and illumination, for example with a slit-lamp biomicroscope . In primary open angle glaucoma, the angle is open in the early stages of disease but later becomes collapsed.
Gonioscopy is an essential tool in evaluating and managing glaucoma. It helps determine the type and severity of glaucoma, as well as guide treatment decisions. By examining the angle, the drainage system of the eye can be assessed and informed decisions regarding medication, laser treatment, or surgery made.
What are conditions need to be differentiated from Primary Open-Angle Glaucoma?
The following conditions present like glaucoma and need to be differentiated from: -
Secondary glaucoma:
Lens luxation
Uveitis
Neoplasia
Haemorrhage.
Uveitis
How is Primary Open-Angle Glaucoma Treated?
Primary open-angle glaucoma (POAG) is a chronic eye condition that typically requires lifelong management. The primary goal of treatment is to lower intraocular pressure (IOP), as high IOP is a major risk factor for the development and progression of POAG. Although there is no cure for glaucoma, the following treatment options are commonly used:
1. Eye Drops: The first-line treatment for POAG involves the use of medicated eye drops. These drops work by either reducing the production of aqueous humor (the fluid inside the eye) or improving its drainage. Commonly prescribed eye drops include
Prostaglandin analogs (e.g., latanoprost 0.005%, travoprost 0.004%) are commonly used 1-3 times daily. Side effects include miosis, break-down of blood-aqueous barrier and conjunctival hyperaemia . They are contraindicated in cases of anterior lens luxation.
Beta-blockers (e.g., timolol 2.5-5%) are usually used 2-3 times daily. Side effects include miosis, bradycardia and hypotension. They can be used in addition to prostaglandin analogues and carbonic anhydrase inhibitors.
Alpha-adrenergic agonists (e.g., Brimonidine, Apraclonidine). They work by reducing the intraocular pressure in patients with open-angle glaucoma or ocular hypertension.
Carbonic anhydrase inhibitors (e.g., dorzolamide 2% and brinzolamide 1%). These agents reduce aqueous humor production by inhibiting carbonic anhydrase within the ciliary epithelium. They are usually used 2-3 times daily and can be added to prostaglandin analogues if intraocular pressure is refractory.
2. Oral Medications: In some cases, oral medications may be prescribed alongside or instead of eye drops to lower IOP. Carbonic anhydrase inhibitors and osmotic agents are examples of oral medications that can be used to manage glaucoma.
3. Laser Trabeculoplasty: Laser trabeculoplasty is a minimally invasive procedure that uses laser energy to improve the drainage of fluid from the eye. It targets the trabecular meshwork, the structure responsible for draining the aqueous humor. By making the meshwork more permeable, laser trabeculoplasty helps reduce IOP. This procedure is typically performed in an outpatient setting and may be repeated if necessary.
4. Filtering Surgery: If eye drops and laser trabeculoplasty are not effective in controlling IOP, a surgical procedure called trabeculectomy may be recommended. During trabeculectomy, a new drainage channel is created to bypass the trabecular meshwork, allowing excess fluid to drain out of the eye. This surgery is usually performed under local anesthesia and requires regular post-operative follow-ups.
5. Drainage Implants: In cases where trabeculectomy is not suitable or has failed, a drainage implant (also known as a glaucoma drainage device or tube shunt) may be considered. These devices are surgically implanted to create a new pathway for fluid drainage, thereby reducing IOP. The implant is typically placed in the front portion of the eye and can be effective in managing glaucoma.
6. Analgesia. Analgesics (pain relievers) are not typically used as a primary treatment for glaucoma, however, some medications may be prescribed to manage associated symptoms or discomfort though these medications do not address the underlying cause of the condition. If a patient with POAG experiences pain or discomfort related to their glaucoma, the treatment approach may involve the use of nonsteroidal anti-inflammatory drugs (NSAIDs) or topical anesthetics to provide temporary relief. NSAIDs used safely in dogs include Vedaprofen, Ketoprofen, Meloxicam, Carprofen, Deracoxib, Firocoxib, Mavacoxib, Robenacoxib and diclofenac (eye drops) can help reduce inflammation and alleviate mild pain or discomfort.
Additionally, topical anesthetics such as tetracaine or proparacaine can also be used to numb the eye temporarily. These anesthetics are usually applied as eye drops before certain procedures or examinations to reduce any potential discomfort.
The choice of treatment depends on several factors, including the severity of the disease, the patient's overall health, and their response to previous treatments. It's essential for patients with POAG to have regular eye examinations and follow recommendations to prevent vision loss or further progression of the condition.
How can Primary Open-Angle Glaucoma be Prevented and Controlled?
DNA testing for known mutations in breeds that are predisposed to them, followed by their removal from the breeding population avoids this inherited disease. The monitoring of canines in risk is also paramount.
What is the Prognosis of Primary Open-Angle Glaucoma?
The initial prognosis is favorable, and with the right treatment, eyes may maintain vision for months to years. In the long run, however, medical therapy frequently fails to maintain normal blood pressure and vision and enucleation is indicated for eyes that remain painful and blind.
References
Kwon, Y. H., Fingert, J. H., Kuehn, M. H., & Alward, W. L. (2009). Primary open-angle glaucoma. New England Journal of Medicine, 360(11), 1113-1124.
Ahonen S J et al (2014) A Novel Missense Mutation in ADAMTS10 in Norwegian Elkhound Primary Glaucoma. PLoS One 9 (11), e111941 PubMed.
Kuchtey J et al (2011) Mapping of the disease locus and identification of ADAMTS10 as a candidate gene in a canine model of primary open angle glaucoma. PLoS Genet 7 (2), e1001306 PubMed.
Pickett J P, Miller P E, & Majors L J (1988) Calibration of the Schiotz tonometer for the canine and feline eyes. Proc Am Coll Vet Ophthalmol 19, 47.
Samuelson D A, Gum G G & Gelatt K N (1989) Ultrastructural changes in the aqueous outflow apparatus of beagles with inherited glaucoma. Invest Ophthalmol Vis Sci 30 (3), 550-561 PubMed.
BSAVA Manual of Ophthalmology. (Eds Gould D & McLellan G). 3rd edition. pp 273-296.
Veterinary Ophthalmology. (Eds Gelatt K, Gilger B, Kern T). 5th edition, pp 1050-1145.
For information on Genetic Testing Providers (labs) genetic tests, and tests by breed, visit International Partnership for Dogs (https://dogwellnet.com/).
For a list of DNA tests available for certain breeds worldwide, visit Kennel Club Worldwide DNA tests: https://www.thekennelclub.org.uk/health/for-breeders/dna-testing-simple-inherited-disorders/worldwide-dna-tests/.
















Comments